Archived Content
The National Institute of Mental Health archives materials that are over 4 years old and no longer being updated. The content on this page is provided for historical reference purposes only and may not reflect current knowledge or information.
Brain Imaging Predicts Psychotherapy Success in Patients with Social Anxiety Disorder
• Science Update
Treatment for social anxiety disorder or social phobia has entered the personalized medicine arena—brain imaging can provide neuromarkers to predict whether traditional options such as cognitive behavioral therapy will work for a particular patient, reported a National Institute of Mental Health (NIMH)-funded study that was published in the January 2013 issue of JAMA Psychiatry.
Background
Social anxiety disorder (SAD)— the fear of being judged by others and humiliated— is the third most prevalent psychiatric disorder in Americans, after depression and alcohol dependence, according to the National Comorbidity Survey, a U.S. poll on mental health. This fear can be so strong that it interferes with daily life activities like going to work or school. If left untreated, some sufferers use alcohol, food, or drugs to reduce the fear at social events, which often leads to other disorders such as alcoholism, eating disorders, and depression. The NIMH claims that 6.8 percent of U.S. adults and 5.5 percent of 13- to 15-year-olds, the age of onset for this chronic disorder, are annually afflicted.
Although psychotherapy and drugs, such as antidepressants and benzodiazepines, exist as treatments for SAD, current behavioral measures poorly predict which would work better for individual patients. “Half of social anxiety disorder patients have satisfactory response to treatment. There is little evidence about which patient would benefit from a particular form of treatment,” said John D. Gabrieli, Ph.D., lead author of the study. “Currently, there is no rational basis for prescribing one treatment over the other. Which treatment a patient gets depends on whom they see.”
Enter personalized medicine, the use of genetic or other biological markers to tailor treatments to those who would actually benefit from them, thus sparing the expense and side effects for those who would not. Brain imaging could identify neuromarkers or targeted areas of the brain that could one day optimize treatment for individual patients. Neuromarkers are being used in other areas of mental illness, for instance, to predict the onset of psychosis in schizophrenia and the likelihood of relapse in drug addiction.
In this study, Gabrieli, at the Massachusetts Institute of Technology in Cambridge, and his colleagues, used functional magnetic resonance imaging (fMRI) in 39 SAD patients before a 12-week course of cognitive behavioral therapy. The patients viewed angry versus neutral faces and scenes while undergoing fMRI examination (see first slide). Compared to neutral faces, angry faces convey disapproval and are likely to prompt excessive fear responses and negative connotations in SAD patients; cognitive behavioral therapy teaches these patients ways to downregulate their responses. The patients’ brain images were then compared to their scores on a conventional clinical measure, the Liebowitz Social Anxiety Scale (LSAS), a questionnaire which they took before and after therapy completion.
Results of the Study
SAD patients responded more to the images of faces and not scenes, which is characteristic for the social basis of this disorder. Patients whose brains reacted strongly to the facial images before treatment benefitted more from the therapy than those who reacted to these the least (see second slide). Specifically, changes in two occipitotemporal brain regions—areas involved in early processing of visual cues such as faces—correlated with positive cognitive behavioral therapy outcome. These neuromarkers predicted treatment outcome better than the currently used LSAS.
Significance
This study is the first of its kind to use neuroimaging to predict treatment response in SAD patients. Neuromarkers may become a practical clinical tool to guide the selection of optimal treatments for individual patients. Integration of neuromarkers with genetic, behavioral, and other biomarkers is likely to further refine the prediction.
What’s Next
A larger study comparing people with SAD with normal participants is needed to verify the results. fMRI studies using other facial expressions (disgust or fear) might be better predictors. Studies that look at other treatment options, such as drugs, are also needed to confirm which treatment is optimal.
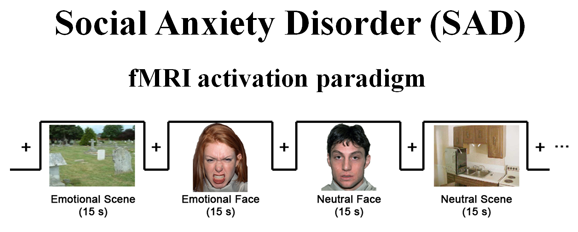
Source: Gabrieli Lab, MIT
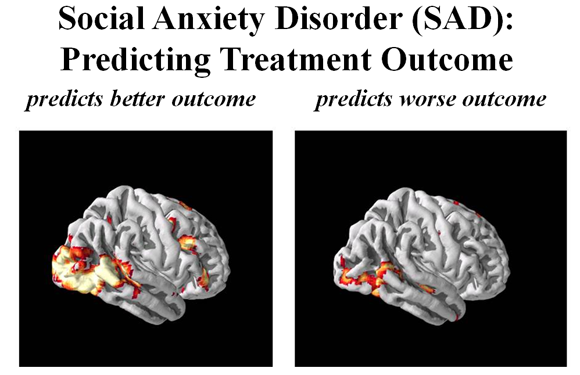
Source: Gabrieli Lab, MIT
Reference
Doehrmann O, Ghosh SS, Polli FE, Reynolds GO, Horn F, Keshavan A, Triantafyllou C, Saygin ZM, Whitfield-Gabrieli S, Hofmann SG, Pollack M, Gabrieli JD. Predicting Treatment Response in Social Anxiety Disorder from Functional Magnetic Resonance Imaging. JAMA Psychiatry. January 2013. 70(1):87–97.
