Archived Content
The National Institute of Mental Health archives materials that are over 4 years old and no longer being updated. The content on this page is provided for historical reference purposes only and may not reflect current knowledge or information.
Same Genes Suspected in Both Depression and Bipolar Illness
Increased Risk May Stem From Variation in Gene On/Off Switch
• Science Update
Protein produced by PBRM1 gene
Researchers, for the first time, have pinpointed a genetic hotspot that confers risk for both bipolar disorder and depression. People with either of these mood disorders were significantly more likely to have risk versions of genes at this site than healthy controls. One of the genes, which codes for part of a cell's machinery that tells genes when to turn on and off, was also found to be over-expressed in the executive hub of bipolar patients' brains, making it a prime suspect. The results add to mounting evidence that major mental disorders overlap at the molecular level.
"People who carry the risk versions may differ in some dimension of brain development that may increase risk for mood disorders later in life," explained Francis McMahon, M.D., of the NIMH Mood and Anxiety Disorders Program, who led the study.
McMahon and an international team of investigators, supported, in part by NIMH, report on the findings of their genome-wide meta-analysis online January 17, 2010 in the journal Nature Genetics.
Background
Major mood disorders affect 20 percent of the population and are among the leading causes of disability worldwide. It's long been known that bipolar disorder and unipolar depression often run together in the same families, hinting at some shared lineage. Yet, until now, no common genes or chromosomal locations had been identified.
McMahon and colleagues analyzed data from five different genome-wide association studies (GWAS) totaling more than 13,600 people, and confirmed their results in 3 additional independent samples totaling 4,677 people.
Findings of This Study
Genetic variations on Chromosome 3 were significantly associated with both mood disorders. The suspect gene, called PBRM1, codes for a protein critical for chromatin remodeling, a key process in regulating gene expression . A neighboring gene is involved in the proliferation of brain stem cells.
The researchers pinpointed a "protective" version of the PBRM1 gene that is carried by 41 percent of healthy controls, but only 38 percent of people with bipolar and unipolar depression. The risk version was found in 62 percent of mood disorder cases and 59 percent of controls. The researchers also showed that PBRM1 is expressed more in the prefrontal cortex of people with bipolar disorder than in controls.
Significance
Since mood disorders likely involve altered gene expression during brain development and in response to stress, PBRM1's profile makes it a good potential candidate gene. This first genetic evidence of unipolar/bipolar overlap is also the first significant genome-wide association with any psychiatric illness in the Chromosome 3p region.
However, the findings underscore limitations of the GWAS approach, which looks for connections to gene versions that are common in the population. Having one copy of this risk variant increases vulnerability for developing a mood disorder by a modest 15 percent. Why do some people with this variant — and presumably other, yet to be discovered, shared risk genes — develop bipolar disorder while others develop unipolar depression or remain healthy? Environmental influences and epigenetic factors may be involved, suggest the researchers, who note that "genetic association findings so far seem to account for little of the inherited risk for mood disorders."
"Our results support the growing view that there aren't common genes with large effects that confer increased risk for mood disorders," said McMahon. "If there were, in this largest sample to date, we would have found them. The disorders likely involve many genes with small effects — and different genes in different families — complicating the search. Rarer genes with large effects may also exist."
What's Next?
Ultimately, findings such as these may lead to identification of common biological pathways that may play a role in both unipolar and bipolar illness and suggest strategies for better treatment, said McMahon. The results add to other evidence of overlap that is spurring a new NIMH initiative to make sense of research findings that don't fit neatly into current diagnostic categories. See: Genes and Circuitry, Not Just Clinical Observation, to Guide Classification for Research.
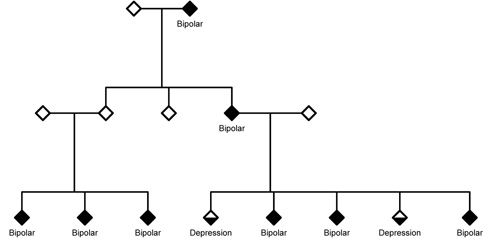
Bipolar disorder and unipolar depression often run in the same families, as this pedigree diagram illustrates. The new study is the first to trace both illnesses to a shared chromosomal hotspot.
Reference
Meta-analysis of genome-wide association data identifies a risk locus for major mood disorders on 3p21.1 .the Bipolar Disorder Genome Study (BiGS) Consortium, McMahon FJ, Akula N, Schulze TG, Muglia P, Tozzi F, Detera-Wadleigh SD, Steele CJ, Breuer R, Strohmaier J, Wendland JR, Mattheisen M, Mühleisen TW, Maier W, Nöthen MM, Cichon S, Farmer A, Vincent JB, Holsboer F, Preisig M, Rietschel M. Nat Genet. 2010 Jan 17. [Epub ahead of print]PMID: 20081856
Samples included in the meta-analysis
dbGaP National Institute of Mental Health bipolar disorder
Genetic Association Information Network MDD
Wellcome Trust Case Control Consortium
German sample
Systematic Treatment Enhancement Program for Bipolar Disorder
