On Being Ill
By
It is cliché to say that doctors make the worst patients. But it is inevitably true that we are always both, though we often forget this. I recently had cause to remember, as those of you who follow my newly established Twitter feed may have already figured out. On Thanksgiving Day, I had the misfortune of breaking my fibula, the smaller of the two bones in the lower leg. Thanksgiving is my favorite secular holiday of the year, as it prioritizes family, celebrates our common American heritage, and gives us pause to be thankful for what we have. My family celebrates it as many do. We watch the big game on TV, play a game of touch football at halftime, and then settle into a boisterous late afternoon feast. This year I didn’t quite make it to the feast. During the halftime event, my competitive spirit outstripped my athletic ability, and down I went, rolling my ankle and cracking the bone straight through.
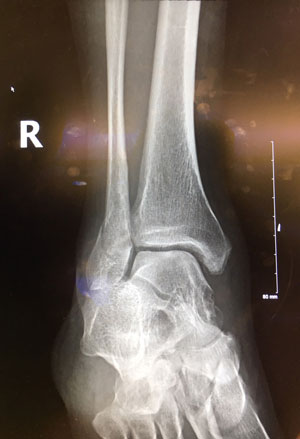
The first thing I felt was pain. Acute, unrelenting, agonizing pain. The second thing I felt was anxiety. I was anxious that I had done something really bad to my ankle that would make my next few months truly challenging. And the third thing I felt, a bit later, was gratitude, as my family gently helped me off the ground and into a car, and drove me to the nearest emergency room.
When I got to the ER a remarkable thing happened. Many of you may have read my September Director’s Message on suicide prevention, where I discussed the value of universal screening for suicide risk. Well, during the intake process, right after asking me what was wrong and while she was taking my blood pressure, the triage nurse asked me whether I was thinking of hurting or killing myself. I said, “No, but thank you for asking!” I was in too much pain to tell her why, but it made me feel great knowing that some ERs have begun to implement this in their routine intake process, even for an over-eager, accidentally injured, amateur athlete like myself.
I didn’t get true relief from the pain until two hours later, when the ER nurse gave me a single pill of acetaminophen and oxycodone, more widely known by its brand name, Percocet. Within 15 minutes my pain was relieved, and I could finally carry out a coherent conversation. Acute pain is something we know how to treat. Someone walks into the ER suffering from excruciating pain, unable talk or even think clearly, and walks out with the pain under control, eager to make it back home to have leftovers with his family and catch the next big game on TV.
Unfortunately, many psychiatric treatments don’t work this way. If you come into the ER suffering from depression and suicidal thoughts, they can give you an antidepressant—but it can take weeks—or even months—for the medicine to help you feel better. Psychotherapies have a similar time course, and even the fastest Food and Drug Administration-approved treatment for depression, electroconvulsive therapy, also typically takes weeks to work. This is why we are really excited about the possibilities of ketamine and related medications currently under development. Ketamine is a novel treatment for depression pioneered by Dr. Carlos Zarate and colleagues here in the intramural program at NIMH. When given intravenously, it can help patients suffering from depression or suicidal thoughts improve in hours, not weeks. While ketamine may not be quite ready for wider use—it has to be administered carefully, with close monitoring; it only works in approximately half of those who get it; its effects last a few days to a week, requiring frequent, time-consuming and expensive repeat treatments; and we don’t know about long-term efficacy and outcomes—the NIMH and others are actively trying to conduct the necessary studies so that one day you might walk into an emergency room with depression, and walk out feeling better, with an appointment to see an outpatient provider to continue your treatment.
I walked out feeling better but with a leg that was still broken and uncertainty about what it would take to fix it. I got an outpatient appointment with an excellent orthopedist, and his cogent explanation of (1) what happened to me, (2) my treatment options and their relative merits, and (3) how long it would take me to recover. This knowledge relieved my anxiety, and two days later I was in the operating room getting the break repaired, with a bit more hardware in my leg and a lot less worry in my brain.
Contrast this reassuring information with what I can provide to my patients as a psychiatrist. I can (1) tell my patients very little about what is wrong with their brains that leads them to suffer, (2) provide them with treatment options but with very little to go on in terms of which treatment might be right for their specific condition, and (3) tell them generally about the long-term prognosis but not give them specific timeframes for recovery. These are the reasons I’m excited about NIMH efforts to define the mechanisms underlying psychiatric illnesses, and precision biomarkers that can guide treatment and inform prognoses.
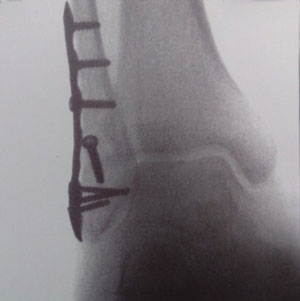
Look closely at the intraoperative x-ray and you’ll also get a sense of the tools available to the orthopedist. Although they are relatively low tech, each of the 7 screws seems to be purposely chosen for length to fit my bone; each angled just so to grip and secure the plate precisely to the bone. The intraoperative x-ray itself is remarkable, allowing the surgeon to verify that my ankle joint was properly aligned before closing me up and sending me on to the recovery room. If only we had such tools in psychiatry. One could argue that some forms of psychotherapies and other psychosocial treatments are indeed specific tools tailored to the patient’s specific problems, and I have certainly used psychotherapy in that fashion. But wouldn’t it be wonderful if we could have the equivalent of an intraoperative x-ray, but aimed at brain function, to see how our therapies were working even while they were being carried out? Wouldn’t it be great to use the biology of the brain to help get even more efficacious treatments and deliver them in a way precisely tailored to the patient? I say the answer to these questions is yes, and that is why I’m excited about the BRAIN Initiative , aimed at developing the necessary tools that will allow us to interrogate brain function in much more specific, comprehensive, and sophisticated ways than current technologies allow.
With the pain and anxiety gone, and my recovery underway, what remains is the gratitude for the health professionals who treated me with dignity and excellence, and for family members, friends, colleagues, and Twitter followers who have directly or indirectly cared for and supported me over the past few weeks. I also recognize, however, that not everyone has the resources and support systems that allow them to access this excellent care, and to recover with the help of their social networks. Individuals suffering from mental illnesses are much less likely to have these resources and supports. Which is why I’m excited about NIMH’s support of research aimed at figuring out how to implement effective care in diverse and under-resourced communities, and to help clarify why those with brain illnesses typically suffer worse outcomes from illnesses in other bodily systems.
A belated Happy Thanksgiving to all of my readers.

